Colorado Health Insurance Marketplace: A Guide to Connect for Health Colorado in 2026
Colorado operates its own state-based health insurance marketplace called Connect for Health Colorado, rather than using the federal HealthCare.gov platform. For the 2026 plan year, 277,228 Coloradans enrolled in medical coverage through the exchange, choosing from plans offered by six private carriers. With a statewide weighted average rate increase above 21% and enhanced federal premium tax credits no longer available, the Colorado health insurance marketplace is navigating its most challenging enrollment environment since the exchange launched in 2013. For a complete overview of all plan types and carrier options, see the Colorado health insurance guide.

What brings you to the Colorado marketplace?
I want to check subsidy eligibility
Federal APTC, CSR, and Colorado Premium Assistance
Check financial help ↓I want to understand the Colorado Option
Standardized plans with $0 copays on the exchange
Explore $0 copay plans ↓I want to know enrollment dates
Open enrollment windows and qualifying life events
See enrollment dates ↓How Connect for Health Colorado Works
Connect for Health Colorado is Colorado’s state-based health insurance marketplace and the only place to access federal premium tax credits and cost-sharing reductions when purchasing individual coverage. For plan year 2026, the exchange enrolled 277,228 Coloradans across plans from six carriers and operates independently from the federal HealthCare.gov platform used by 29 other states.
Unlike the states that rely on HealthCare.gov, Colorado’s exchange operates its own enrollment platform with its own tools, including the Estimate & Explore feature that lets consumers compare plans by premium, deductible, and estimated total annual cost based on expected healthcare use. Connect for Health Colorado also runs a separate dental marketplace that enrolled more than 80,000 Coloradans in dental coverage during the 2025 open enrollment period. Free enrollment assistance is available through a statewide network of more than 900 certified Assisters and licensed agents in 22+ languages.
The exchange also operates the Colorado Connect platform, which provides marketplace access for undocumented immigrants through the OmniSalud program. For 2026, OmniSalud enrollment is limited to 6,700 spots on a lottery basis due to state funding cuts.
Financial Help for Colorado Health Insurance Marketplace Plans in 2026
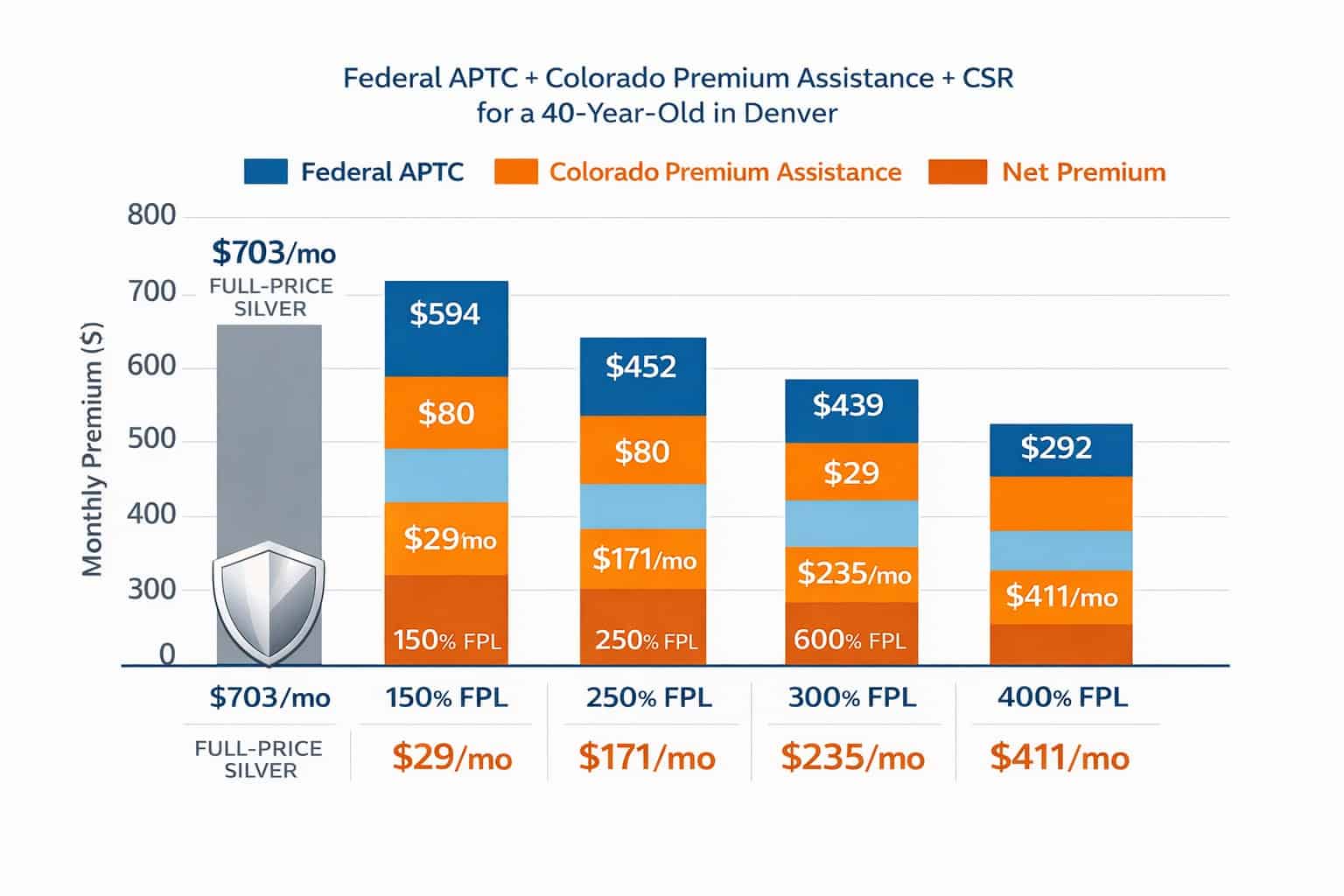
69% of Connect for Health Colorado enrollees received financial assistance in 2026 through three stacking programs: federal Advanced Premium Tax Credits, cost-sharing reductions for Silver plan enrollees below 250% FPL, and Colorado Premium Assistance providing $80 per month for the primary applicant and $29 per month for each additional family member.
The amount of help dropped significantly after enhanced federal premium tax credits expired on December 31, 2025. Colorado responded by creating the Colorado Premium Assistance program with approximately $100 million in one-time state funding, which provides $80 per month for the primary applicant and $29 per month for each additional family member for households earning up to 400% of the federal poverty level ($62,400 for an individual, $128,600 for a family of four). For a full breakdown of cost strategies and how different income levels affect net premiums, see the affordable health insurance in Colorado guide.
Federal Advanced Premium Tax Credits (APTC) remain available for households between 100% and 400% FPL, calculated against the benchmark Silver plan in the enrollee’s county. Cost-sharing reductions (CSR) lower deductibles and copays for enrollees below 250% FPL who select a Silver-tier plan on the exchange.
| Income Level (Individual) | Federal APTC | CO Premium Assistance | CSR Eligible |
|---|---|---|---|
| 150% FPL (~$22,590) | Yes, large credit | $80/month | Yes (Silver plan) |
| 250% FPL (~$37,650) | Yes, moderate credit | $80/month | Yes (Silver plan) |
| 300% FPL (~$45,180) | Yes, smaller credit | $80/month | No |
| 400% FPL (~$62,400) | Yes, minimal credit | $80/month | No |
| Above 400% FPL | No | No | No |
Colorado Premium Assistance: Sunset Risk
Colorado Premium Assistance is funded by a one-time $100 million state appropriation for 2026 only. The program’s future depends on legislative action and should not be treated as a permanent benefit when planning multi-year coverage decisions.
Example: Subsidy Stacking for a Denver Family of Four at 250% FPL ($75,300/Year)
The family qualifies for a federal APTC of approximately $950/month, Colorado Premium Assistance of $167/month ($80 primary + $29 × 3 dependents), and cost-sharing reductions on a Silver plan. Their net monthly premium for a Silver Colorado Option plan is approximately $180, compared to $2,360/month at full price. Without the state supplement, the same family would pay roughly $347/month.
Check Your Colorado Marketplace Subsidy Eligibility
69% of Connect for Health Colorado enrollees received financial help for 2026. Enter your ZIP code and household income to see your estimated 2026 premium after all available subsidies.
Colorado Option Plans on the Marketplace
The Colorado Option is a standardized plan design available exclusively through Connect for Health Colorado that requires $0 copays for primary care, mental health visits, diabetic supplies, and prenatal and postnatal care. During the 2025 open enrollment period, 47% of all marketplace enrollees selected a Colorado Option plan, up from 34% in 2024 and just 14% in its first year in 2023.
All six individual market carriers on the Colorado health insurance marketplace must offer Colorado Option plans at the Bronze, Silver, and Gold tiers in every county where they sell coverage. The standardized benefit design means that a Kaiser Colorado Option Silver plan and an Anthem Colorado Option Silver plan have identical copay structures; the differences are limited to provider network, geographic availability, and premium price. Starting in 2026, the Colorado Division of Insurance caps Colorado Option premium increases at the medical inflation rate and can hold public hearings to set reimbursement rates if carriers miss premium reduction targets.
For marketplace shoppers comparing plans, the Colorado Option simplifies the decision. Instead of analyzing different copay and deductible structures per carrier, consumers can focus on two variables: which doctors and hospitals are in each carrier’s network, and what the monthly premium costs after subsidies. More than half of subsidy-eligible marketplace enrollees had at least one Colorado Option plan with an estimated net premium under $10/month in 2025.
2026 Open Enrollment and Special Enrollment in Colorado
Open enrollment for 2026 Connect for Health Colorado coverage ran from November 1, 2025 through January 15, 2026. Enrollees who selected a plan by December 15 received coverage effective January 1. Outside of open enrollment, Colorado offers a 60-day special enrollment period following qualifying life events, including pregnancy, which Colorado has recognized as a qualifying event since 2024.
Connect for Health Colorado offers a 60-day special enrollment period following qualifying life events. Colorado recognizes the standard federal qualifying events: job loss, marriage, birth or adoption, moving to a new county, and losing other coverage. It also adds a provision unique to the state: since 2024, pregnancy is a qualifying life event. Uninsured pregnant Coloradans can enroll in marketplace coverage at any time without waiting for open enrollment or giving birth first. This pairs directly with Colorado Option plans’ $0 prenatal and postnatal care copays.
Coverage Loss
Losing employer coverage, aging off a parent’s plan at 26, COBRA expiration, or a Medicaid/CHP+ eligibility change. 60-day enrollment window from the event date.
Life Changes
Marriage, divorce, birth or adoption of a child, or death of a covered family member. 60-day window from the event date.
Relocation
Moving to a new Colorado county or moving to Colorado from another state. Carrier options and premiums change by county. Denver metro has 6 carriers while mountain counties may have only 1 or 2.
Pregnancy (Colorado-Specific)
Since 2024, pregnancy qualifies as a special enrollment event in Colorado, one of only a handful of states with this provision. Connects directly to Colorado Option $0 prenatal and postnatal copays.
Metal Tiers and Plan Comparison on Connect for Health Colorado
Connect for Health Colorado offers plans at four metal tiers: Bronze, Silver, Gold, and Platinum. Silver plans are the most popular tier because they are the only plans eligible for cost-sharing reductions and serve as the benchmark for federal subsidy calculations. For a 40-year-old in Denver, 2026 premiums before subsidies range from approximately $390/month for Bronze to $710/month for Gold.
Connect for Health Colorado’s Estimate & Explore tool allows shoppers to input their expected healthcare use (doctor visits, prescriptions, planned procedures) to generate an estimated total annual cost per plan, not just the monthly premium. This is particularly useful in Colorado’s marketplace where the same Silver tier can range from $520/month to $940/month depending on whether the enrollee lives in Denver or a mountain resort community. For a detailed carrier-by-carrier comparison including quality ratings and network strengths, see the best health insurance in Colorado guide.
| Tier | Actuarial Value | Avg. Denver Premium (40-yr-old) | Best For |
|---|---|---|---|
| Bronze | 60% | ~$390/mo | Low premiums, healthy individuals, HSA pairing |
| Silver | 70% (up to 94% with CSR) | ~$590/mo | CSR-eligible enrollees, moderate care use |
| Gold | 80% | ~$710/mo | Frequent care users, ongoing prescriptions |
| Platinum | 90% | Limited availability | Maximum coverage, lowest per-visit costs |
On-Exchange vs. Off-Exchange Plans in Colorado
Enrolling through Connect for Health Colorado is required to access federal premium tax credits and cost-sharing reductions. Consumers above 400% FPL who do not qualify for subsidies should compare off-exchange plans from Anthem and Cigna, where Silver plans avoid cost-sharing reduction loading and can cost $30–$50 less per month than equivalent on-exchange options. For self-employed Coloradans and independent buyers, see the individual health insurance Colorado guide.
Colorado residents can purchase ACA-compliant health insurance through the Colorado health insurance marketplace or directly from carriers off-exchange. The core tradeoff is straightforward: on-exchange enrollment is required to access premium tax credits and cost-sharing reductions, but off-exchange plans from Anthem and Cigna include PPO options that provide out-of-network flexibility not available from every on-exchange plan.
For consumers earning above 400% FPL ($62,400 individual) who do not qualify for any financial assistance, off-exchange plans can offer better value at the Silver tier. On-exchange Silver plans carry cost-sharing reduction loading (an inflated premium that funds CSR benefits for lower-income enrollees) while off-exchange Silver plans do not carry this loading. In Denver, an Anthem off-exchange Silver PPO can cost $30–$50 less per month than the equivalent on-exchange Silver HMO, with better network flexibility. For more on PPO-specific options available off-exchange, see the Colorado PPO health insurance guide.
Consumers below 400% FPL should almost always enroll on-exchange. Even a modest federal APTC of $50/month, combined with the $80/month Colorado Premium Assistance, outweighs any off-exchange pricing advantage. A licensed agent can run a side-by-side comparison for both pathways to determine the break-even income point.
On-Exchange vs. Off-Exchange Decision Rule
If household income is below 400% FPL, enroll through Connect for Health Colorado to access subsidies. If income is above 400% FPL, compare off-exchange Anthem and Cigna PPO pricing against on-exchange options. The off-exchange Silver tier typically offers better value without CSR loading.
Frequently Asked Questions About the Colorado Health Insurance Marketplace
Common questions about the Colorado health insurance marketplace in 2026 focus on how Connect for Health Colorado differs from HealthCare.gov, what financial help is available after enhanced federal subsidies expired, whether to buy on-exchange or off-exchange, and how pregnancy qualifies as a special enrollment event.
Is Connect for Health Colorado the same as HealthCare.gov?
No. Colorado operates its own state-based exchange called Connect for Health Colorado. Residents enroll through connectforhealthco.com, not HealthCare.gov. The exchange has its own enrollment platform, carrier selection (6 carriers for 2026), and tools including the Estimate & Explore plan comparison feature. Colorado is one of 21 states (plus D.C.) that runs a state-based marketplace.
What is Colorado Premium Assistance and who qualifies?
Colorado Premium Assistance is a state-funded program providing $80/month for the primary applicant and $29/month for each additional family member on a marketplace plan. Households earning up to 400% FPL qualify. The program was created during a 2025 special session with $100 million in one-time state funding and stacks on top of any federal premium tax credits.
Can I enroll in a Colorado marketplace plan if I am pregnant?
Yes. Since 2024, Colorado recognizes pregnancy as a qualifying life event for special enrollment. Uninsured pregnant Coloradans can enroll through Connect for Health Colorado at any time, with no need to wait for open enrollment or to give birth first. Colorado Option plans then cover prenatal and postnatal care with $0 copays.
How many carriers are on the Colorado marketplace in 2026?
Six carriers offer medical plans through Connect for Health Colorado for 2026: Anthem Blue Cross Blue Shield, Cigna, Denver Health Medical Plan, Kaiser Permanente, Rocky Mountain Health Plans, and SelectHealth. Availability varies by county. Denver metro has all six, while mountain and Western Slope communities may have only one or two.
Should I buy on-exchange or off-exchange in Colorado?
If household income is below 400% FPL, enroll on-exchange through Connect for Health Colorado to access federal tax credits and Colorado Premium Assistance. If income is above 400% FPL, compare off-exchange PPO plans from Anthem and Cigna. The Silver tier is often cheaper off-exchange because it avoids cost-sharing reduction loading.
Colorado Health Insurance Resources
Complete overview of all plan types, carriers, and 2026 market changes.
Affordable Coverage OptionsCost breakdowns, subsidy strategies, and Colorado Premium Assistance details.
Best Health Insurance in ColoradoCarrier comparisons, quality ratings, and network details for all 6 carriers.
Colorado PPO PlansPPO carrier comparisons, on vs. off-exchange options from Anthem and Cigna.
Individual Health InsuranceSelf-employed coverage, off-exchange options, and plan selection for Coloradans.
PPO Health Insurance PlansCompare PPO plans nationwide, including options from Anthem and Cigna.
Compare Colorado Marketplace Plans for 2026
See plan options and pricing from all six Connect for Health Colorado carriers in your county. Check your subsidy eligibility and find the best plan for your budget.
Broker Disclosure
ForHealthInsurance.com is an independent health insurance agency serving Colorado residents. We are not affiliated with any carrier or government agency. We help you compare plans and enroll in coverage that meets your needs at no extra cost to you.