Kentucky Health Insurance Marketplace: kynect 2026 Plans & Enrollment
The Kentucky health insurance marketplace — officially called kynect — is the state’s own exchange, separate from HealthCare.gov, where residents shop for individual and family coverage, check subsidy eligibility, and apply for Medicaid. This guide covers how the Kentucky health insurance marketplace works in 2026, which carriers are available in your county, and how to enroll or change plans.

What do you need help with?
What Is kynect and How Does It Work?
Kynect is the Kentucky health insurance marketplace — one of roughly 18 states that operate their own exchange rather than using HealthCare.gov. In 2026, approximately 89,000 Kentuckians enrolled through kynect, down from 97,000 in 2025 after enhanced federal subsidies expired. Kynect offers plans from three carriers, handles subsidy applications, and provides access to Medicaid and KCHIP enrollment year-round.
Kentucky’s exchange has a unique backstory. Governor Steve Beshear launched kynect in 2013, and it became one of the most successful state exchanges in the country. Governor Matt Bevin deactivated it in 2017, shifting Kentuckians to HealthCare.gov. Governor Andy Beshear relaunched kynect in 2022 — making Kentucky the only state to have shut down and restarted its own exchange. Today, kynect is fully operational at kynect.ky.gov and serves as the single portal for marketplace plans, Medicaid, KCHIP, and other benefits programs.
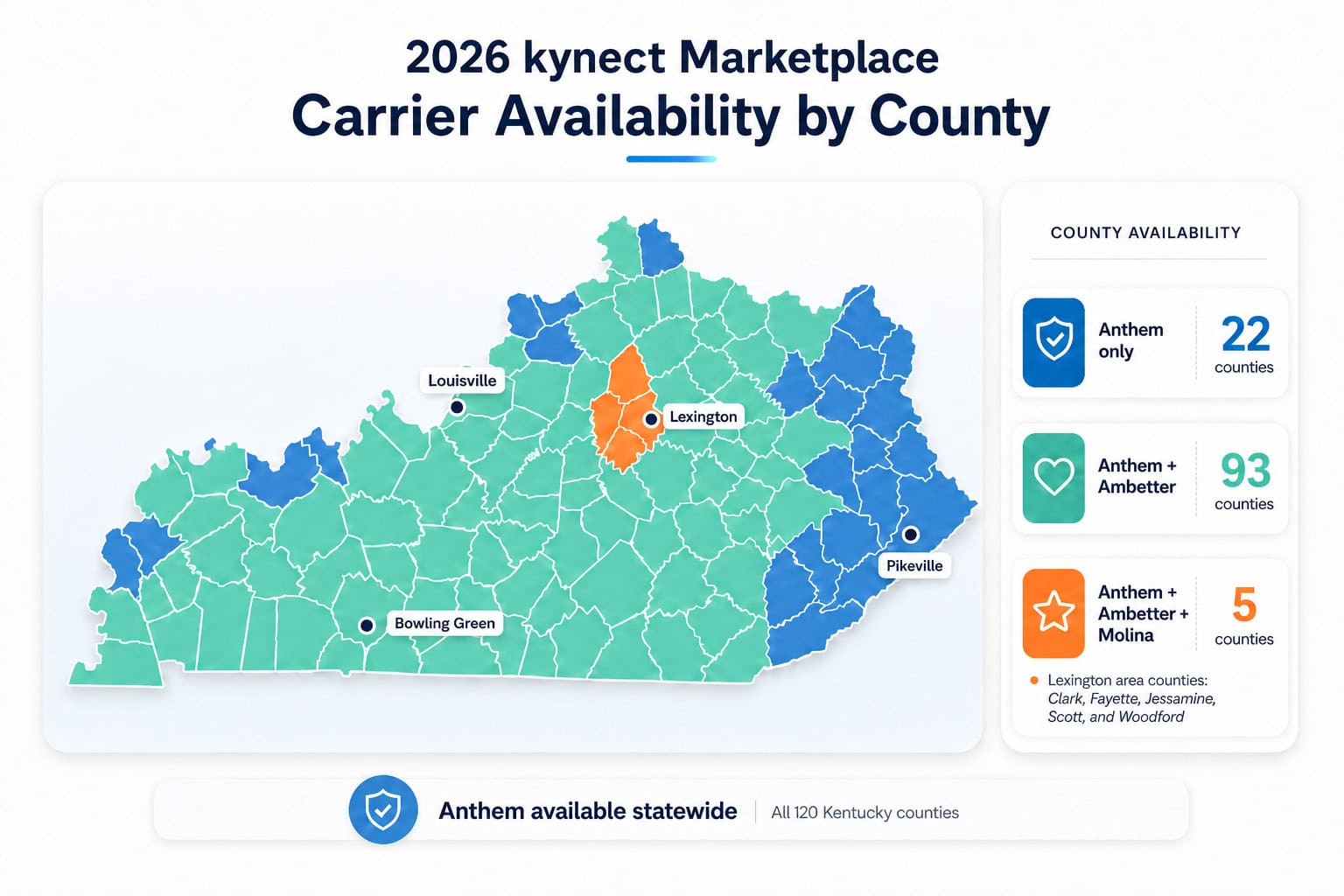
Unlike HealthCare.gov states, kynect has its own enrollment platform and a statewide network of certified enrollment assisters called kynectors. Licensed agents can show both kynect plans and off-exchange Anthem options that kynectors cannot access. Ambetter by WellCare of Kentucky covers 108 counties. Passport Health Plan by Molina is available in only 5 counties around Lexington (Clark, Fayette, Jessamine, Scott, Woodford). Roughly 22 Kentucky counties have only Anthem as a marketplace option.
| Carrier | Counties Served | Plan Types | Notable |
|---|---|---|---|
| Anthem Blue Cross Blue Shield | All 120 counties (Pathway); 48 counties (Transition) | Pathway HMO, Transition (broader network) | Only carrier with statewide coverage; Transition includes Baptist Health, Norton, UK HealthCare |
| Ambetter by WellCare of Kentucky | 93 counties | HMO | Lowest Silver premiums (~$617/mo age 40); condition-specific plans for asthma/COPD in 2026 |
| Passport Health Plan by Molina Healthcare | 5 counties (Clark, Fayette, Jessamine, Scott, Woodford) | HMO | Lexington area only; cheapest Silver in Fayette County (~$521/mo age 40) |
CareSource, which had been Kentucky’s fourth marketplace carrier, stopped offering individual plans at the end of 2025. This contraction hit rural eastern Kentucky hardest — counties like Breathitt, Harlan, Letcher, and Owsley now have only Anthem as a marketplace option. Kentuckians in single-carrier counties should compare Anthem’s Pathway (lower cost, narrower network) against Transition plans (higher cost, broader access to facilities like Appalachian Regional Healthcare).
Anthem’s Pathway Transition plans — which offer the broadest network in the individual market, including Baptist Health, Norton Healthcare, and UK HealthCare — are available in only 48 of Kentucky’s 120 counties. Transition plans are not available in most rural eastern Kentucky counties, where smaller hospitals are outside the Transition network. For a detailed comparison of Anthem’s network tiers and off-exchange options, see the Best Health Insurance in Kentucky guide.
Subsidies and Financial Help on kynect in 2026
Premium tax credits are available to Kentucky residents enrolling through the Kentucky health insurance marketplace with household incomes between 100% and 400% of the Federal Poverty Level — roughly $15,960 to $62,600 for a single adult in 2026. Enhanced subsidies in place since 2021 expired at the end of 2025, resulting in smaller credits and no subsidy eligibility above 400% FPL. In 2025, 86% of Kentucky enrollees received subsidies averaging $489/month; 2026 subsidies are smaller.
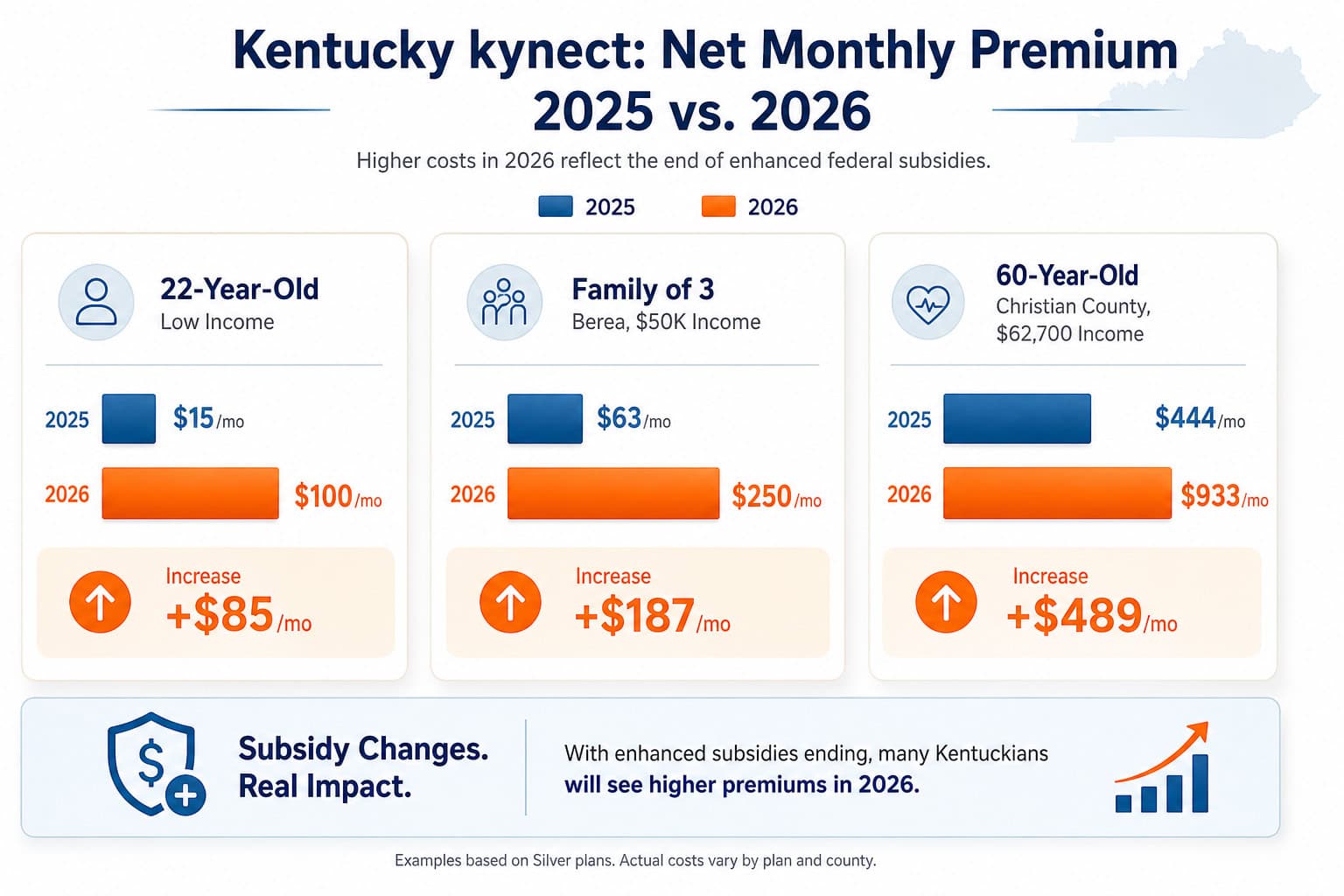
The subsidy expiration hit Kentucky enrollees particularly hard. Analysis from the Kentucky Center for Economic Policy shows average out-of-pocket cost increases of $181–$200/month, with some households seeing spikes of 60%–600%. A 22-year-old low-income enrollee saw net premiums rise from approximately $15/month to $100/month. A 60-year-old small business owner in Christian County earning $62,700/year — just above the new subsidy cutoff — saw premiums nearly double from $444 to $933/month.
Cost-sharing reductions (CSRs) are still available in 2026 for Kentucky residents who select Silver plans through kynect with incomes up to 250% FPL (~$39,900 single adult). CSR plans reduce deductibles and out-of-pocket maximums beyond what the premium credit covers. In 2025, 48% of Kentucky marketplace enrollees selected Silver plans with built-in CSR benefits — the most effective way to reduce total out-of-pocket costs at lower income levels.
Subsidy check is free on kynect: Kentucky residents can check their subsidy eligibility by visiting kynect.ky.gov and completing a prescreening — no full application required. A licensed enrollment assistant at ForHealthInsurance.com can run a full subsidy estimate at no cost — including off-exchange Anthem comparisons. Call 888-215-4045.
How to Enroll Through kynect — Step by Step
Kentucky residents enroll through the Kentucky health insurance marketplace at kynect.ky.gov during Open Enrollment (November 1 – January 15). Enrolling by December 15 starts coverage January 1; enrolling December 16 – January 15 starts coverage February 1. Approximately 89,000 Kentuckians selected marketplace plans during the 2026 OEP. Enrollment requires proof of income, Social Security numbers for household members, and Kentucky residency. Medicaid and KCHIP enrollment is open year-round.
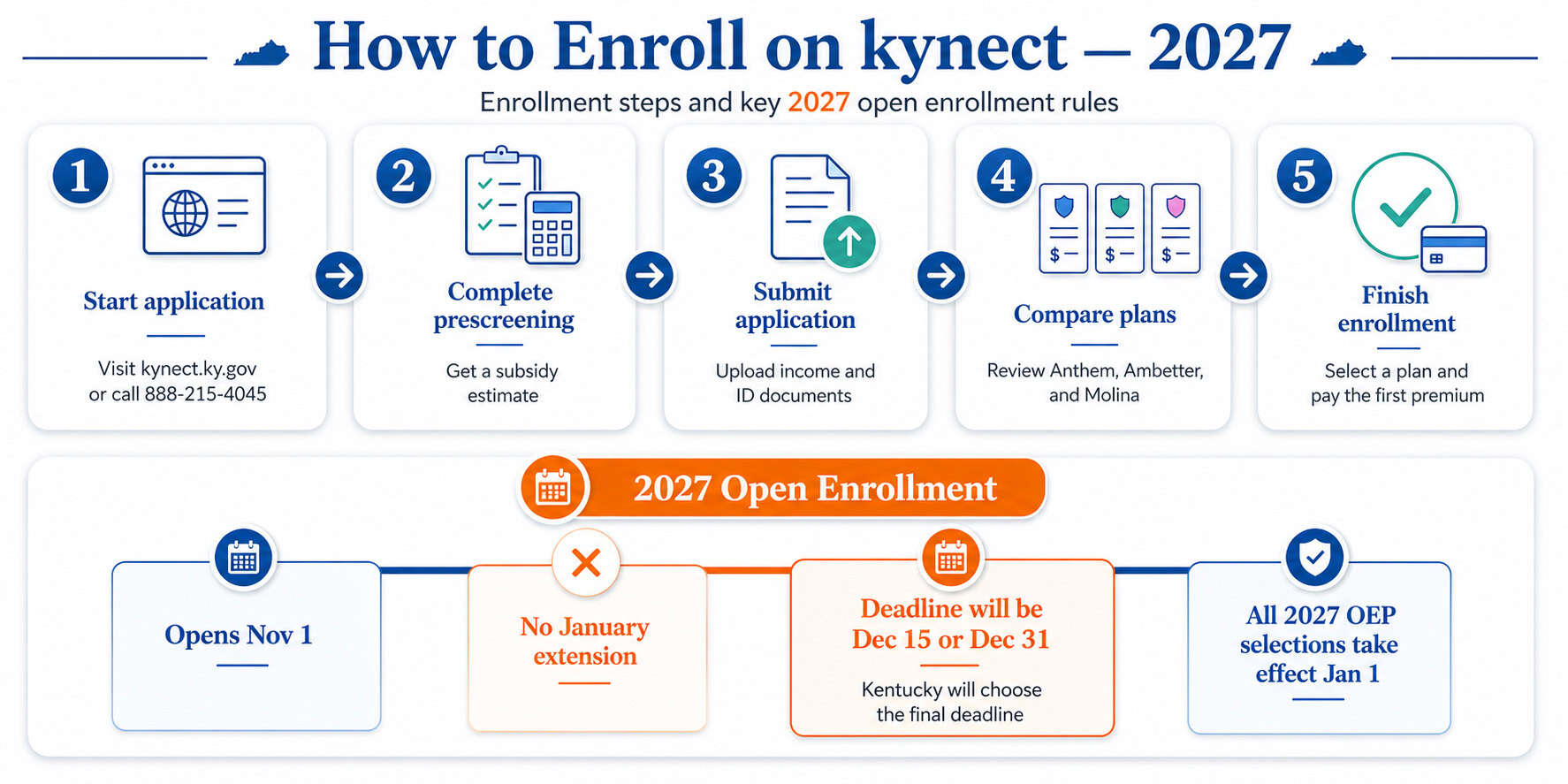
You’ll need Social Security numbers for everyone in your household, proof of income (pay stubs, tax returns, or self-employment records), and immigration documentation if applicable. Have your current health insurance information ready if switching plans.
Start at kynect.ky.gov or call ForHealthInsurance.com at 888-215-4045 for a free guided enrollment. Licensed enrollment assistants can provide free enrollment help — including Medicaid and KCHIP screening, kynect plan comparison, and off-exchange Anthem options.
Kynect lets you prescreen before submitting a full application. Enter your household size and estimated income to see whether you qualify for Medicaid, KCHIP, or premium tax credits — and get an estimate of your monthly costs before committing.
Kynect displays all available plans in your county with premium, deductible, and network details. Enter your zip code to see whether Anthem, Ambetter, and/or Molina serve your area. Use the Plan Comparison Tool to compare up to three plans side by side.
Coverage does not start until the first premium payment is received by the carrier. Expect a member ID card within 2–3 weeks. Confirm your effective date: December 15 enrollment starts January 1; January 15 enrollment starts February 1.
2027 enrollment change ahead: Starting with the 2027 plan year, kynect’s open enrollment will end no later than December 31 — it will no longer continue into January. Kentucky will decide whether to end enrollment on December 15 (matching HealthCare.gov states) or December 31. All plans selected during the 2027 OEP will take effect January 1.
Special Enrollment Periods and Year-Round Options
Outside of open enrollment on the Kentucky health insurance marketplace, a qualifying life event (QLE) opens a 60-day Special Enrollment Period on kynect. Kentucky Medicaid and KCHIP enrollment is open year-round — no qualifying event needed. American Indian and Alaska Native residents can also enroll in Kentucky health insurance marketplace plans at any time. In 2025, enrollment fell roughly 8% (from 97,000 to 89,000) — meaning more Kentuckians may need SEP options mid-year as costs become clearer.
Lost job-based coverage
Job loss or COBRA expiration triggers a 60-day SEP on kynect. Compare a subsidized Silver plan against COBRA — COBRA averages ~$702/month in Kentucky, while a subsidized kynect plan often costs significantly less.
Moved to or within Kentucky
Moving to Kentucky from another state, or between Kentucky counties, triggers an SEP. Important: carrier availability varies by county — a move from Fayette County (3 carriers) to Harlan County (1 carrier) changes your options.
Marriage, divorce, or new child
Getting married, divorced, or having/adopting a child triggers a 60-day SEP. A new baby or adopted child can be added to an existing kynect plan or enrolled in KCHIP if the family qualifies.
Lost Medicaid eligibility
Kentucky residents who lose Medicaid (e.g., income rising above 138% FPL) trigger a kynect SEP. With HB 2 (enacted April 2026) introducing community engagement requirements for ~478,900 expansion adults, more Kentuckians may transition from Medicaid to marketplace plans mid-year.
Kentuckians who fall outside an SEP window but still need coverage between jobs or while waiting for the next OEP have two non-marketplace options: Kentucky short-term health insurance (limited to 4 months total under federal rules effective September 2024) or off-exchange Anthem plans, which are sold year-round but are not subsidy-eligible. To compare 2026 kynect premiums against off-exchange and short-term alternatives for your county, request Kentucky health insurance quotes through a licensed enrollment assistant at no cost.
Need Help Enrolling on kynect?
Compare kynect marketplace plans, check your subsidy eligibility, and enroll with a licensed enrollment assistant — no cost, no obligation.
Kynectors, Agents, and Free Enrollment Help
The Kentucky health insurance marketplace offers two types of free enrollment assistance: kynectors (state-certified enrollment assisters funded by KHBE, available in all 120 counties) and licensed insurance agents who can access both kynect marketplace plans and off-exchange options. Kynectors helped thousands of Kentuckians enroll during the 2026 OEP — particularly in rural eastern Kentucky counties where internet access and health literacy barriers are highest.
Kynectors are unique to Kentucky — the term comes from the kynect platform itself, and they serve a similar role to federally funded “navigators” in HealthCare.gov states. The key difference: kynectors are certified by the Kentucky Health Benefit Exchange (KHBE) and trained specifically on the kynect enrollment system, Medicaid, and KCHIP applications. They cannot recommend a specific plan, but they can walk Kentuckians through the application, explain subsidy results, and help compare options.
Licensed insurance agents can do everything a kynector can, plus show off-exchange plans from Anthem that are not visible on kynect. For Kentuckians earning above the subsidy threshold ($62,600 single adult), an agent can compare kynect plans against off-exchange Anthem Transition plans to find the lower-cost option. There is no extra cost for using an agent — carrier commissions cover the service. ForHealthInsurance.com serves Kentucky residents at 888-215-4045.
Get free enrollment help: A licensed enrollment assistant at ForHealthInsurance.com can compare kynect and off-exchange plans at no cost. Call 888-215-4045. Kynectors are available year-round — not just during open enrollment.
On-Exchange vs. Off-Exchange Plans in Kentucky
Plans purchased through the Kentucky health insurance marketplace (kynect) are eligible for premium tax credits and cost-sharing reductions. Off-exchange plans are sold directly by Anthem and are not eligible for subsidies, but may carry lower base premiums for Kentuckians above the subsidy threshold — because off-exchange Silver plans don’t include cost-sharing reduction loading that inflates on-exchange Silver pricing. In 2026, the subsidy cutoff at 400% FPL ($62,600 single adult) makes this comparison especially relevant.
For Kentucky residents who qualify for subsidies (under $62,600 single adult), enrolling through kynect is almost always the better option — the premium tax credit applies only to on-exchange plans. But for those above the subsidy threshold, comparing Anthem’s off-exchange Transition plans against on-exchange Silver plans is worth the effort. A licensed enrollment assistant can run both quotes side by side to show the net cost difference. For a full carrier comparison including off-exchange pricing, see the Best Health Insurance in Kentucky guide.
Frequently Asked Questions About kynect
Common kynect Kentucky health insurance marketplace questions for 2026 cover whether kynect replaces HealthCare.gov in Kentucky, the 3-carrier kynect lineup after CareSource exited at the end of 2025, the November 1 to January 15 open enrollment window, special enrollment periods after qualifying life events, free kynector availability across all 120 Kentucky counties, and how the 15.1%–37% rate increases affect the ~89,000 enrolled Kentuckians.
Is kynect the same as HealthCare.gov?
No. Kynect is Kentucky’s own state-based marketplace at kynect.ky.gov — it is separate from HealthCare.gov. Kentucky briefly used HealthCare.gov from 2017 to 2021 but relaunched kynect for the 2022 plan year. All Kentucky marketplace enrollment now goes through kynect, not the federal site.
How many carriers are on kynect for 2026?
Three carriers: Anthem Blue Cross Blue Shield (all 120 counties with Pathway plans; 48 counties with Transition plans), Ambetter by WellCare of Kentucky (108 counties), and Passport Health Plan by Molina (5 Lexington-area counties: Clark, Fayette, Jessamine, Scott, Woodford). CareSource exited the Kentucky marketplace at the end of 2025, reducing the carrier count from four to three.
What is a kynector and how do I find one?
A kynector is a state-certified enrollment assister trained on the kynect platform. Licensed enrollment assistants provide free help with marketplace applications, Medicaid enrollment, and KCHIP — and can also show off-exchange Anthem plans. A licensed enrollment assistant at ForHealthInsurance.com can provide the same kynect enrollment help plus off-exchange plan comparison — call 888-215-4045.
Can I enroll outside of open enrollment on kynect?
Marketplace plan enrollment outside of OEP (November 1 – January 15) requires a qualifying life event such as losing job-based coverage, getting married, having a child, or moving to a new Kentucky county. The Special Enrollment Period lasts 60 days from the qualifying event. Kentucky Medicaid and KCHIP enrollment is open year-round — no qualifying event needed.
Why did my kynect premiums increase so much for 2026?
Two factors: base rate increases of 15.1%–37% across carriers, and the expiration of enhanced federal premium tax credits at the end of 2025. The enhanced subsidies had kept out-of-pocket costs low since 2021. Without them, subsidies cover less of the total premium, and households above 400% FPL ($62,600 single adult) lost subsidy eligibility entirely. Enrollees are seeing net cost increases averaging $181–$200/month.
Should I use kynect or buy directly from a carrier?
If your income is under $62,600 (single adult), enroll through kynect — premium tax credits and cost-sharing reductions are only available on-exchange. If your income is above the subsidy threshold, compare kynect plans against off-exchange Anthem Transition plans — the off-exchange option may cost less because it doesn’t carry cost-sharing reduction loading. A licensed enrollment assistant can run both quotes at no cost.
Kentucky Health Insurance Resources
2026 pillar guide — kynect, Kentucky Medicaid, KCHIP, HB 2 reforms, and the ~89,000 Kentucky enrollees
Best Health Insurance in KentuckyCompare all 3 carriers — Anthem, Ambetter by WellCare, Passport by Molina — with Kentucky county coverage
Affordable Health Insurance KentuckyKentucky Medicaid, KCHIP, premium tables, and how HB 2 affects 478,900 expansion adults
Individual Health Insurance KentuckyCoverage for self-employed Kentuckians, Bluegrass farm operators, and residents above the $62,600 subsidy cutoff
Kentucky Health Insurance QuotesCompare 2026 kynect, off-exchange Anthem, and short-term quotes side by side for any Kentucky county
PPO Health Insurance PlansCompare PPO options nationwide — flexible provider access, no referrals required, in and out of network
Ready to Enroll on kynect?
Compare 2026 kynect plans from Anthem, Ambetter by WellCare, and Passport by Molina, check your subsidy eligibility against the $62,600 (400% FPL) cutoff, and enroll with free help from a licensed enrollment assistant — joining the ~89,000 Kentuckians on kynect for 2026.
Broker Disclosure
ForHealthInsurance.com is an independent health insurance agency serving Kentucky residents. We are not affiliated with any carrier or government agency. We help you compare plans and enroll in coverage that meets your needs at no extra cost to you.